Hair follicles, mainly at the hairline and forehead, are affected by the confusing and frequently upsetting condition known as frontal fibrosing alopecia. We will examine the different aspects of frontal fibrosing alopecia as we delve into this thorough guide, providing insight into its definition, causes, symptoms, diagnosis, and available treatments.
2. What is Frontal Fibrosing Alopecia?
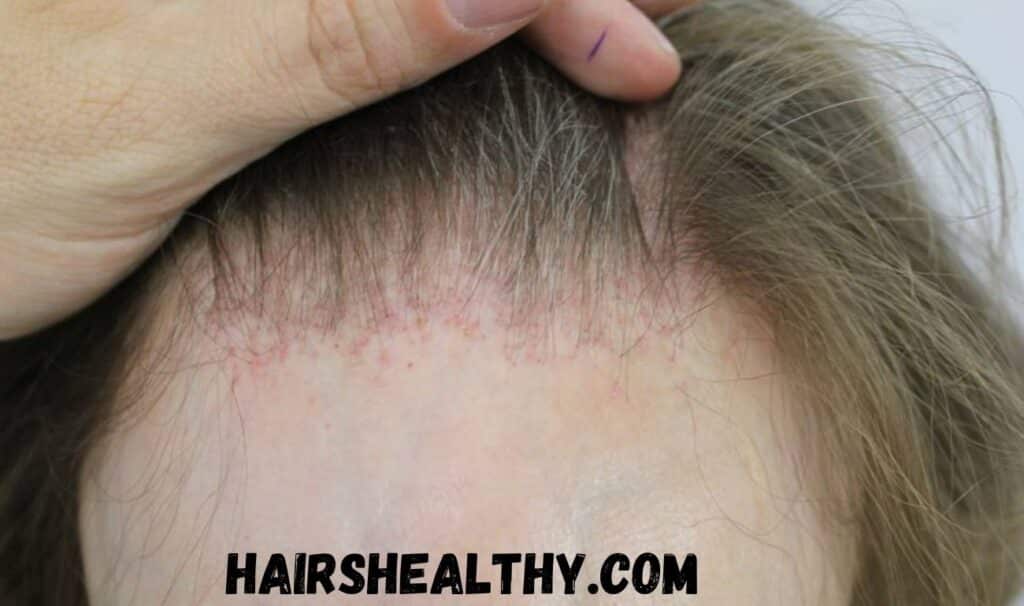
A type of scarring hair loss called frontal fibrosing alopecia (FFA) mostly affects the eyebrows and frontal hairline. It is a rather uncommon ailment, and nobody knows for sure what causes it. Although it can also affect men and premenopausal women, FFA is more frequently seen in postmenopausal women.
Progressive recession of the frontal hairline, frequently combined with eyebrow hair loss, is the defining characteristic of FFA. There may be visible scarring in the affected areas, which appear smooth and pale. Sometimes the scalp may also show signs of redness and inflammation.
The reason behind frontal fibrosis Although the exact causes of alopecia are unknown, a mix of genetic, hormonal, and environmental factors are thought to be involved. Genetic predisposition, autoimmune reactions, and hormonal changes are thought to have a role in the development of FFA.
3. Who might have Frontal Fibrosing Alopecia?
The majority of cases of frontal fibrosing alopecia (FFA) are seen in postmenopausal women, usually in the age range of 50 to 70. Nonetheless, it can impact people of all ages, including men and women who are not yet menopausal. The precise cause of FFA is unknown, and it is thought to be relatively uncommon.
Frontal Fibrosing Alopecia may arise as a result of a number of factors, such as hormonal fluctuations, genetic predisposition, and possibly autoimmune processes. Given that FFA is more common in postmenopausal women, some studies raise the possibility of a hormonal component. However, the illness can also strike people in whom there is no obvious hormonal component.
Although FFA primarily affects the eyebrows and frontal hairline, it can affect other parts of the scalp as well.
4. How common is Frontal Fibrosing Alopecia?
Although frontal fibrosing alopecia (FFA) is still regarded as a relatively uncommon condition, over time, its prevalence has been rising. The recent identification of FFA as a unique clinical entity may have contributed to its rarity by raising awareness and facilitating diagnosis.
There are regional and population-based differences in the prevalence of FFA. Especially in women of European descent, postmenopausal women are more likely to report having the condition. Cases, however, have been reported in people of different ages, genders, and ethnicities.
5. Causes of Frontal Fibrosing Alopecia?
Although the precise causes of Frontal Fibrosing Alopecia (FFA) are unknown, a combination of genetic, hormonal, and environmental factors are most likely to be responsible. The following elements could play a role in the development of FFA:
Genetic Predisposition: Given that FFA often impacts people with a family history of autoimmune diseases or hair loss disorders, it appears to have a genetic component. There may be certain genetic factors that increase an individual’s risk of developing FFA.
Hormonal Factors: Hormonal changes could be involved, especially in postmenopausal women, who account for a large number of FFA cases. Hormonal fluctuations, particularly decreased estrogen levels following menopause, may play a role in the development of FFA. But our understanding of the precise hormonal mechanisms at play is still lacking.
Autoimmune Processes: FFA is thought to exhibit autoimmune features, in which the immune system of the body unintentionally targets and destroys hair follicles. Hair loss is the ultimate result of this immune response, which also causes inflammation and scarring. It’s still unknown what precisely sets off the autoimmune reaction in FFA.
Environmental Factors: According to certain research, environmental variables like exposure to specific chemicals or pollutants may have a role in the development of FFA. To definitively link environmental factors to the onset of the condition, more research is necessary.
Inflammatory Processes: One common characteristic of FFA is chronic inflammation of the scalp. Hair follicle damage and scarring due to the inflammatory response may result in permanent hair loss.
6. Symptoms of Frontal Fibrosing Alopecia?
The symptoms of frontal fibrosing alopecia (FFA) are distinct and mainly affect the frontal hairline and eyebrows. Although each person’s symptoms may differ, the condition is progressive and common features include:
Recession of the Frontal Hairline: One of the hallmark signs of FFA is the gradual recession of the frontal hairline. Over time, the hairline moves backward, creating a widening and more pronounced forehead.
Eyebrow Hair Loss: FFA often leads to the loss of eyebrow hair, which can be a distinguishing feature. This may involve the entire eyebrow or specific parts of it.
Smooth and Pale Skin: The affected areas of the scalp may appear smooth and pale due to scarring. The skin in these areas may lack hair follicles and exhibit signs of damage.
Redness and Inflammation: Some individuals with FFA may experience redness and inflammation of the scalp. This can contribute to discomfort and is indicative of the inflammatory nature of the condition.
Itching or Burning Sensations: Patients with FFA may report sensations of itching or burning on the scalp. These symptoms can vary in intensity and may contribute to the overall discomfort associated with the condition.
Hair Loss Beyond the Hairline: While FFA primarily affects the frontal hairline and eyebrows, it can extend to other areas of the scalp, leading to generalized hair loss in some cases.
Thinning of Sideburns and Temporal Hair: FFA may also involve the sideburns and temporal areas, leading to thinning or complete loss of hair in these regions
7. How is Frontal Fibrosing Alopecia Diagnosed?
A combination of the clinical assessment, medical history, and occasionally additional testing is used to diagnose frontal fibrosing alopecia (FFA). An outline of the FFA diagnostic procedure is provided below:
Clinical Examination: A dermatologist will conduct a thorough examination of the affected areas, including the frontal hairline, eyebrows, and other regions of the scalp. They will look for signs of hair loss, scarring, and inflammation. The characteristic features of FFA, such as a recession of the frontal hairline and loss of eyebrow hair, are key diagnostic indicators.
Medical History: The dermatologist will inquire about the patient’s medical history, including any family history of hair loss, autoimmune diseases, or skin conditions. Details about the onset and progression of symptoms, as well as any relevant factors like hormonal changes or environmental exposures, may be discussed.
Scalp Biopsy: In some cases, a scalp biopsy may be performed to confirm the diagnosis. During a biopsy, a small sample of the affected scalp tissue is taken for examination under a microscope. This helps in assessing the presence of inflammation, scarring, and other histological features characteristic of FFA.
Blood Tests: Blood tests may be ordered to rule out other potential causes of hair loss and to check for autoimmune markers. While there is no specific blood test for FFA, certain markers may help in understanding the overall health of the patient and identifying potential contributing factors.
Photographic Documentation: Taking photographs of the affected areas during different stages of the condition can aid in tracking the progression of FFA and assessing the effectiveness of treatment over time.
8. How is Frontal Fibrosing Alopecia Treated?
There is no known cure for frontal fibrosing alopecia (FFA), making it a difficult condition to treat. Nonetheless, a number of treatment modalities seek to control symptoms, impede the disease’s advancement, and, in certain situations, encourage regrowth. Based on the patient’s response to various interventions and the severity of their symptoms, treatment plans are frequently customized. The following are some typical FFA treatment options:
Topical Corticosteroids: High-potency topical corticosteroids are frequently prescribed to reduce inflammation and slow down the progression of FFA. These medications are applied directly to the affected areas of the scalp.
Systemic Corticosteroids: In some cases, oral corticosteroids may be prescribed to control inflammation and halt the progression of FFA. However, long-term use of systemic corticosteroids is generally avoided due to potential side effects.
Topical Calcineurin Inhibitors: Tacrolimus and pimecrolimus are topical calcineurin inhibitors that may be used as alternatives or adjuncts to corticosteroids. They help modulate the immune response and reduce inflammation.
Oral Antimalarial Medications: Hydroxychloroquine, an antimalarial drug, has been used in the treatment of FFA due to its anti-inflammatory properties. It may be prescribed in combination with other medications.
Isotretinoin: This medication, commonly used for acne, has been explored as a potential treatment for FFA. Its exact mechanism in treating FFA is not well understood, and further research is needed.
Hormone Replacement Therapy: In postmenopausal women, hormone replacement therapy (HRT) may be considered to address hormonal imbalances that could contribute to FFA. However, the use of HRT is a subject of ongoing research and should be carefully evaluated on a case-by-case basis.
Hair Regrowth Treatments: Minoxidil, a topical medication commonly used for Male pattern hair loss, may be considered to promote regrowth in some individuals with FFA. It may not work for everyone and tends to be more effective in the early stages of the condition.
Finasteride (Propecia®) or dutasteride, taken as a pill to prevent more hair loss.
9. Conclusion
The end will provide a comprehensive summary of frontal fibrosing alopecia by summarizing the main ideas covered in this article. After reading this, readers will have a better knowledge of the illness and the resources available to help them manage and cope with it.
Can frontal fibrosing alopecia be reversed?
Unfortunately, there is no known cure for frontal fibrosing alopecia. However, early intervention and appropriate management can help slow down its progression.
Is frontal fibrosing alopecia hereditary?
Research suggests a potential genetic component, but the exact hereditary nature of frontal fibrosing alopecia is not fully understood.
Can stress trigger frontal fibrosing alopecia?
While stress is believed to play a role in some cases, the exact relationship between stress and frontal fibrosing alopecia is complex and varies among individuals.